Continuous airway positive pressure
Table of Contents
Table of Contents
Continuous positive airway pressure therapy (CPAP) is a well-known treatment for people suffering from sleep apnea. It involves the use of a machine to deliver constant air pressure through a mask worn over the nose or mouth during sleep. However, there are ethical considerations that come with this treatment, which need to be addressed for better patient care.
Pain Points
Patients often experience discomfort while using CPAP equipment, including dry throat and mouth, skin abrasions, mask discomfort, and general claustrophobia. On the other hand, medical professionals can face ethical dilemmas when patients do not follow treatment protocols, requiring the healthcare provider to make decisions about continuing care even with non-compliant patients.
Target of CPAP and Professional Ethics
The target of CPAP is to improve the quality of life of individuals who suffer from sleep apnea. However, healthcare professionals administering CPAP treatment must balance the benefits with the risks. Medical professionals must also receive continuous education on the ethical considerations involved in patient care, such as promoting patient autonomy, benevolence, fidelity, and non-maleficence.
Main Points
The CPAP treatment is a non-invasive procedure used to reduce systematic health risks such as strokes, heart attacks, and other health conditions related to sleep apnea. Despite the efficacy of the treatment, discomfort and ethical considerations such as the duty of care, informed consent, and patient rights are factors that medical professionals need to consider in caring for patients undergoing CPAP therapy.
CPAP and Professional Ethics
CPAP therapy is a medical treatment that requires the collaboration of healthcare professionals and patients to work effectively. Medical professionals must ensure that patients get the proper care, and patients must do their part in adhering to the treatment regimen. Despite the challenges, healthcare practitioners must maintain ethical standards in the delivery of care by upholding the principles of autonomy, beneficence, non-maleficence, and justice in patient care.
 ### Ethics in CPAP Therapy
### Ethics in CPAP Therapy
Ethics plays a vital role in CPAP therapy. Medical professionals must make informed decisions on patient care and respect the patient’s autonomy. A good example is the provision of informed consent before starting the therapy. Patients must also understand that they have the right to refuse treatment. Medical professionals must uphold honesty and transparency in communication, ensuring that patients understand the risks and benefits of the treatment before consenting.
 #### Importance of Ethical Considerations
#### Importance of Ethical Considerations
CPAP therapy is not just about providing relief to sleep apnea patients. Medical professionals must consider every aspect of patient care, including ethics. By upholding ethical principles, medical practitioners will ensure that patients trust them and give them the confidence to follow the treatment regimen. By addressing ethical considerations, the patients are more likely to complete treatment, which would lead to better health outcomes.
Question and Answer
Q: Is it necessary to provide informed consent before starting CPAP therapy?
A: Yes, it is crucial to provide informed consent before starting CPAP therapy. The patient should understand the benefits and risks of the treatment to make an informed decision about what is best for them.
Q: Can ethical considerations impact the success of CPAP treatment?
A: Yes, ethical considerations can impact the success of CPAP treatment. Patients who feel that their autonomy has been respected by medical professionals are more likely to follow the treatment regimen, leading to better health outcomes.
Q: Is it ethical to continue CPAP therapy for patients who do not follow the treatment regimen?
A: The ethical dilemma arises when patients do not follow the treatment regimen. Healthcare providers need to make decisions about continuing care, even with non-compliant patients. The healthcare practitioners should ensure that the patients understand the risks and benefits of the treatment and provide proper education and resources to increase compliance.
Q: Does the duty of care extend to follow-up visits and post-treatment care?
A: Yes, the duty of care extends to follow-up visits and post-treatment care. Medical professionals must ensure that patients get the proper care even after completing the treatment. Ensuring continuity of care is essential in upholding the principles of beneficence and non-maleficence.
Conclusion of CPAP and Professional Ethics
In conclusion, the success of CPAP treatment involves more than just providing relief to patients with sleep apnea. Healthcare professionals must address the ethical considerations involved in patient care, such as patient autonomy, informed consent, and duty of care, to ensure that patients receive the best care possible. Similarly, patients must understand and follow the treatment regimen, which will lead to better health outcomes and improve their quality of life.
Gallery
Continuous Positive Airway Pressure Therapy | Nursing Information

Photo Credit by: bing.com / pressure continuous positive airway therapy
Mechanism Of Action Of Continuous Positive Airway Pressure Therapy IV

Photo Credit by: bing.com / airway mechanism
Positive Airway Pressure Therapy For Heart Failure
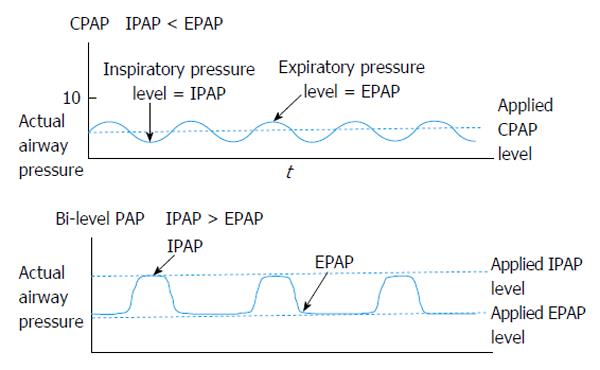
Photo Credit by: bing.com / pressure airway positive continuous bi level therapy 1175 wjc heart failure v6 i11
What Is Continuous Positive Airway Pressure Therapy? | GenesisCare

Photo Credit by: bing.com / continuous airway positive pressure
Continuous Positive Airway Pressure (CPAP) Devices Market

Photo Credit by: bing.com / pressure positive airway continuous cpap devices types market machine breathing bipap different insights premium press release



